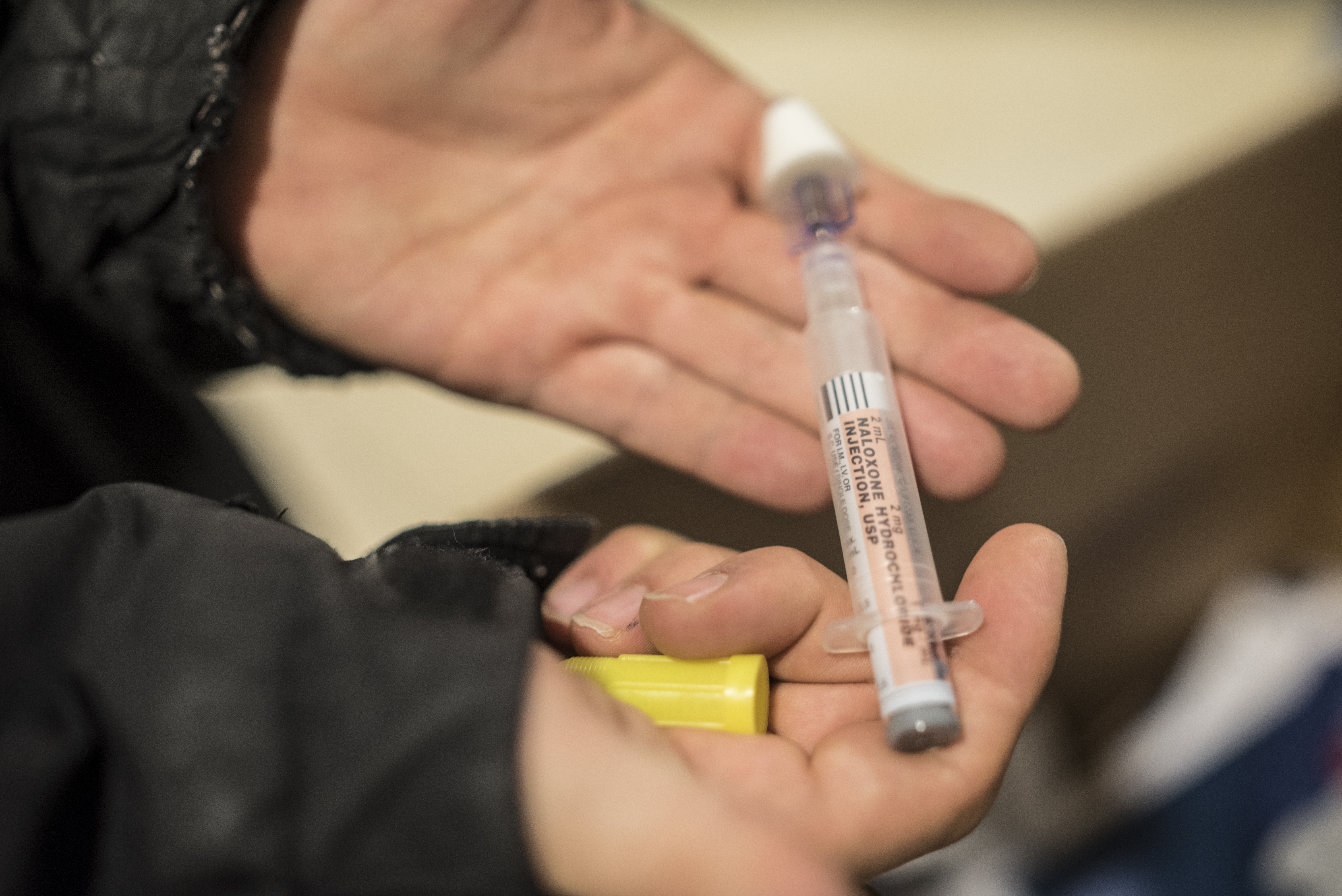
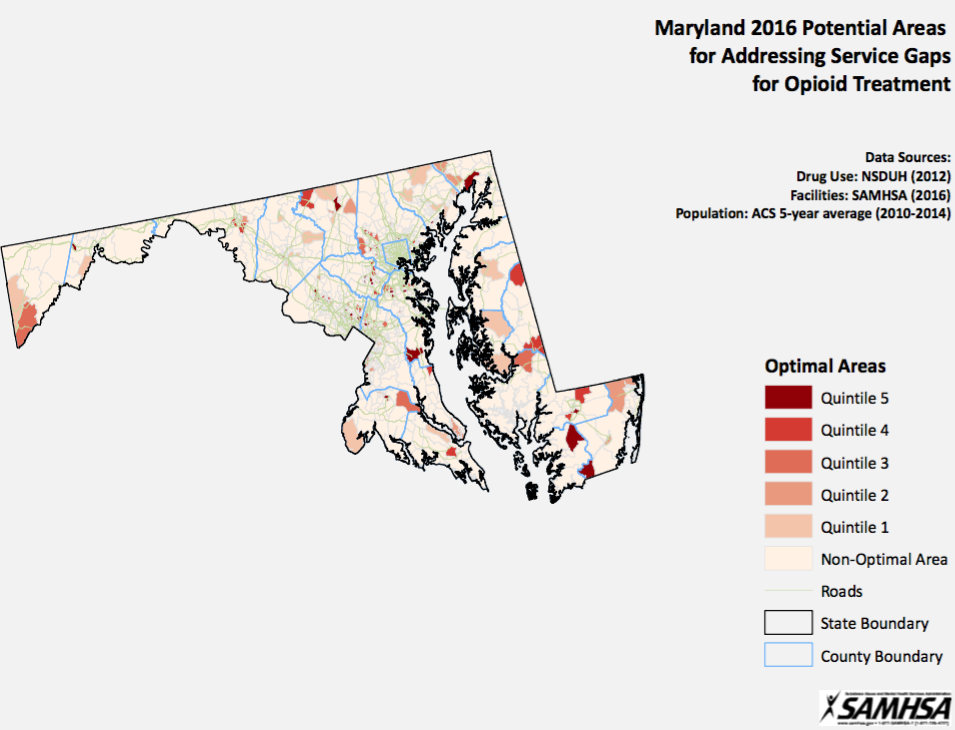
Nationally, opioid prescribing patterns and an increasing use of illicit heroin and fentanyl have contributed to what has been termed an “opioid crisis” or “opioid epidemic”. While opioid use has been around for decades, and has historically been viewed through the lens of the criminal justice system, the term “epidemic” signifies a shift in national thought. As opioid addiction has moved beyond low-income, minority and mostly urban neighborhoods and now cuts across all geographic, demographic and socio-economic boundaries, opioid use disorders are increasingly viewed as a public health concern, requiring a comprehensive, multi-pronged approach to address the underlying causes of addiction, as well as supply chain interdiction.
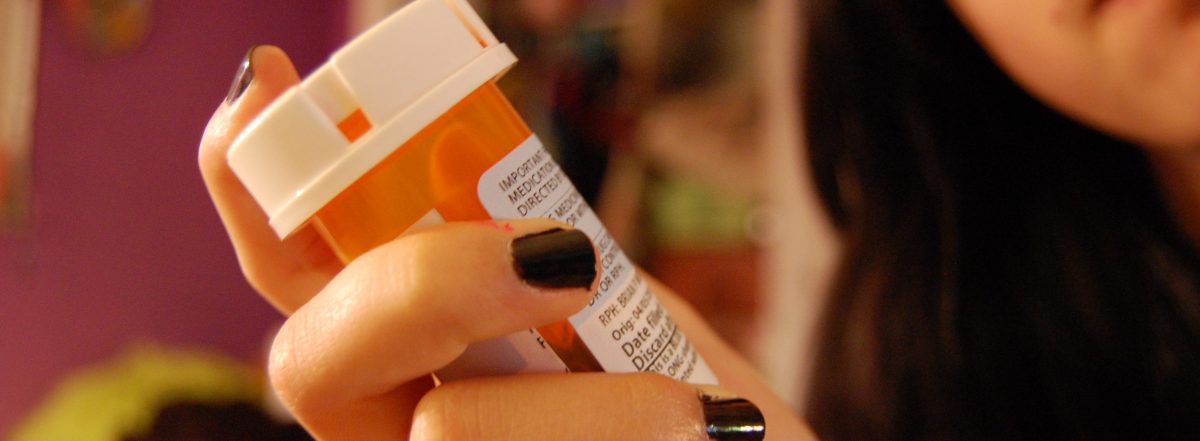
Prescription Opioid Epidemic
A combination of factors led to inappropriate opioid prescribing patterns and quadrupled sales of prescription opioids since 1999. In 1980, a one-paragraph letter from a doctor in a Boston hospital was published in the New England Journal of Medicine, asserting that addiction to opioids is exceedingly rare in hospitalized patients with no history of addiction. For years, pharmaceutical companies cited the letter in marketing the drugs directly to prescribers, asserting that prescription painkillers were a safe way to manage pain with minimal risk of addiction. In 1996, the American Pain Society introduced the concept of pain as a fifth vital sign, despite the fact that there is no objective way to measure pain. In 2001, the Joint Commission, a nonprofit that sets standards and accredits hospitals and medical centers, established assessing pain in all patients as a priority. The Centers for Medicare & Medicaid Services (CMS) administers several patient experience surveys, one of which, the Hospital Consumer Assessment of Healthcare Providers & Systems (HCAHPS) survey, affects Medicaid and Medicare payments. Under value-based purchasing initiatives, hospitals with higher scores receive higher reimbursement rates from CMS. With respect to a growing opioid crisis, three of the survey’s questions were of particular concern: if patients needed medication for pain during their stay, how often their pain was well controlled, and whether the hospital staff did everything they could to help with the pain.
Although these standards and surveys were designed to elevate the issue of pain management and did not explicitly tell doctors to prescribe opioids for pain, there is evidence that hospitals put additional pressure on doctors to aggressively treat pain. Independent studies have suggested that 28% of doctors are paid bonuses based on HCAHPS results, and one in five doctors reported that their jobs were placed in jeopardy as a result of low scores. The CDC has since released new guidelines for doctors prescribing opioids for pain, and CMS is eliminating pain-related questions from HCAHPS surveys as of October 2017. However, for many patients who have since developed opioid dependencies as a result of medical care, the damage has already been done.
Besides poorly-aligned incentives, physicians and other providers are often not well-equipped to present patients with a complete range of pain management options. There are no full residency training programs in pain medicine in the United States. Further, pre- and post-graduate training in pain management and opioid prescription is limited for general practitioners and specialists in family or internal medicine, and continuing medical education courses are often sponsored by pharmaceutical manufacturers who have promoted the use of opioids for pain management. Generally, there is a lack of research on how to treat pain effectively. Though some alternatives to opioids for chronic pain exist, like biofeedback, acupuncture, cognitive behavioral therapy, and alternative physical therapies, even if providers are aware of them, health insurers often exclude certain treatments from coverage. In response to the dramatic rise in prescription-related opioid addiction across the United States, HHS has released a National Pain Strategy, outlining the federal government’s plan for addressing the prevalence of chronic pain in more appropriate ways.